Depression and Addiction
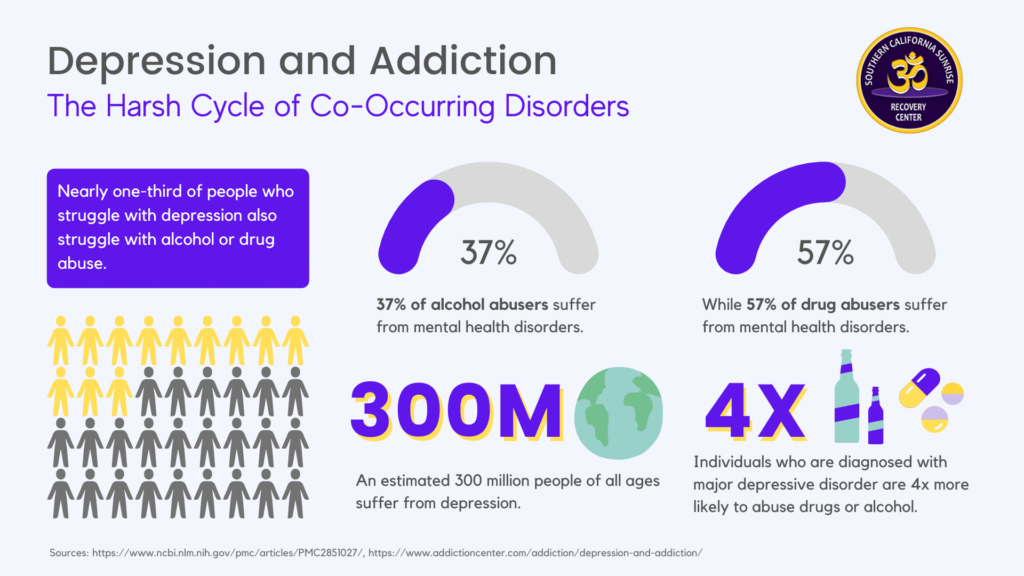
Depression and addiction can go hand in hand. Almost 1/3 of people who are clinically depressed engage in drug or alcohol abuse. Substance abuse can often be a form of self-medication for individuals battling mental health disorders like depression. Fortunately, addiction treatment centers like ours offer dual diagnosis treatment to treat co-occurring disorders.
Table of Contents
Depression treatment isn’t one-size-fits-all. For severe, persistent, or treatment-resistant symptoms, residential care for depression provides an intensity and structure that outpatient programs can’t match, including 24/7 support, integrated psychiatric care, and evidence-based therapies under one roof.
If you’re looking for help for depression and addiction, you’re not alone. Unfortunately, 1 in 10 Americans will face substance use disorder at some point in their lives, and the same amount will experience depression every year. This co-occurrence underscores the urgency of seeking comprehensive treatment options that address both mental health and substance use issues simultaneously.
Because they are so common, many people have experienced both illnesses simultaneously. Luckily, that means that there is help available. Many specialized treatment programs focus on dual diagnosis, ensuring individuals receive integrated therapy and support for a more effective path toward recovery.
Let’s talk about how to help someone with depression and addiction. By recognizing the signs early, connecting with qualified mental health professionals, and establishing a strong support system, it becomes possible to break the cycle of these co-occurring disorders and move toward lasting wellness.
What Is Depression?
Before we jump into finding depression help for a loved one, we need first to define what depression is, as there are common misconceptions about the illness.
Depression is not just “having the blues” or being sad. The happiest people in the world feel sad sometimes, and that’s no reason for concern.
Instead, depression is a serious illness where the brain can no longer produce normal levels of essential neurotransmitters like serotonin, throwing off the normal chemical balances in your brain, which leads to a host of issues related to both physical and mental health.
The condition forms and displays differently for every person, and it can cause serious complications, including permanent brain damage, when left untreated. While depression requires a medical diagnosis, most people will understand if they have it just by reflecting.
Having “low” periods, experiencing feelings of numbness, harmful or suicidal thoughts, and a sense of hopelessness are common with depression. Again, everybody experiences sadness, but it becomes depression when these feelings don’t go away on their own.
Understanding how the two conditions affect one another is essential to knowing how to help. Let’s discuss this.
The Link Between Addiction and Depression
Substance use disorder (SUD) does not necessarily have to be coupled with depression or another mental health disorder. SUD is a mental health disorder itself.
However, the two have been linked on numerous occasions due to the large number of patients suffering from them simultaneously.
When people with depression experience some of the extreme symptoms mentioned above, it is common for patients to self-medicate, which is a dangerous practice that often leads to addiction when left untreated. If the pain or numbness doesn’t go away on its own, people will make difficult choices if they don’t see another way.
Self-medication, when left untreated, leaves the potential for long-term brain damage, chronic health conditions, worsening addiction, and overdose. The longer these conditions are left untreated, the more dangerous it is for that person and those around them.
Neither depression nor SUD necessarily causes the other. Taking this on a case-by-case basis is often highly recommended.
However, for people who have experienced depression (or another mental health disorder) for long periods or even most of their lives, substance abuse may be used as a coping mechanism.
Common examples include people who grew up in a traumatic environment and never found treatment for their mental illness and entered adulthood or their teenage years looking for an escape.
For those who developed an addiction before the onset of depression, substances take a high toll on the body. In many cases, drugs take the place of certain neurotransmitters, flooding the brain with them and leading to a positive “high.”
When this happens, our bodies decrease the production of these neurotransmitters, which often leads to depression.
For example, drugs like cocaine (or even alcohol) are chemically similar to the neurotransmitter dopamine, which is the compound associated with pleasure. When your brain is flooded with (what it perceives as) synthetic dopamine, your body shuts off the production of dopamine, which can lead to depression.
Recognizing Depression and Addiction
Unfortunately, nobody wears the word “depressed” on their forehead, and depression will manifest differently from person to person. Somebody can wear a smile on their face every day, go out and engage in recreational activities, hold down a job, and more while still being depressed. Because of this, it is often challenging to recognize depression in others.
However, if you know the person well, you may be able to spot when they are acting out of the ordinary or changing their behaviors, which can make it easier to recognize.
Fortunately, there are ways to recognize addiction in others, but they aren’t perfect.
For example, if somebody is constantly:
- Lying about whereabouts
- Running out of money
- Stealing money
- Using their prescriptions quickly
- Drinking excessively
- Behaving erratically
- Spending time with the wrong people
- Getting sick
These are likely signs of addiction when added together. If this is the case, then you may want to step in and help, but you need to know how to do it correctly to avoid worsening the situation.
How To Help Someone with Depression & Addiction
It is a difficult task to convince somebody who may feel apathetic about their very existence that they need help, which is why prying and badgering won’t be effective in most cases.
However, if you are concerned for somebody who you believe to have a persistent mental health disorder and SUD, there are ways you can help. Here is how to start.
Intervene
First, you need to talk to them, but you need to do it effectively. Interventions are an excellent tool when performed correctly, but they can cause major regressions without proper care.
If you choose to intervene, you must prepare your statements ahead of time and ensure that there is no hostility involved. The best interest of the person struggling should be the only priority in every line of the prepared statements. If you aren’t sure about something, don’t use it.
Interventions are not a time to air out dirty laundry. If you want to yell at them, save it for another time or don’t do it at all. The first sign of hostility is likely to make the person either blow up or walk out.
Remember that interventions are highly emotional events, so be careful with your wording, tone, and message. You are trying to help them, after all.
In terms of messaging, don’t simply focus on how they hurt you, as this will only make them feel worse.
Instead, your messaging should be to remind them of their future, the things they have to look forward to, and how much better their life will be with the proper treatment. Remember that it’s very difficult to recognize this on your own with depression.
Have Options Prepared
There are many potential solutions for addiction and other mental health conditions, so do your research to find the right programs.
If your intervention is successful and your loved one is willing to consider treatment options, having options prepared for them ahead of time will help. Don’t give them time to change their mind.
In order to do this, you will need a special type of treatment that takes into account their mental health disorder as well as their SUD. A traditional rehab program is not enough to address the root cause of their issues, so it’s important to find the right program for their needs and that accepts their insurance.
Finding Help For Addiction and Depression
The trick about treating addiction and depression is that one can’t be treated without the other. If the depression is treated but the addiction isn’t, then the addiction is likely to cause a “relapse” in depression.
Consequently, if the addiction is treated and the depression persists, these feelings of hopelessness and apathy will cause serious complications on the journey to recovery. Recovery is a difficult process fraught with many obstacles, so a clear mind and a willingness to live a healthy lifestyle are important.
Because of this, people struggling with a mental health disorder and addiction require special assistance for the best outcomes. Let’s talk about that.
Dual diagnosis treatment is specialized treatment for those with an existing mental health disorder coinciding with addiction. These programs attempt to address the route cause of addiction and other conditions and develop an appropriate treatment plan for each patient.
Again, treating one without the other is a recipe for disaster, so the right treatment program is important to the success of each individual.
- Medication
- Family therapy
- Individual therapy
- Specialized support groups
- Medical treatments
The list goes on during the rehab stages. Patients with a dual diagnosis will attend similar meetings and events to other patients but will have more personalized treatment plans available to them.
There is a common misconception about rehab that it is a “one and done” process that completely heals you. This is a dangerous belief, and it’s one of the reasons why even the best facilities have relapse rates between 40% and 60%.
Recovery is an ongoing process, especially when there are other underlying conditions like depression, which means that treatment will need to persist long after rehab for the best results.
Treatments will likely include a 12-step program, which is standard after inpatient treatment, along with ongoing medication treatments, therapy, and doctor visits.
Ongoing treatment will look different for every patient but it is necessary, especially during early recovery, to prevent relapse and develop healthy habits and routines.
There are plenty of lifestyle changes that are critical to a successful recovery for anybody recovering from SUD. However, it’s even more critical with the addition of a mental health disorder.
First, a critical lifestyle change to make is cutting out toxic relationships from your life. People who feed into addiction or depressive thoughts and feelings have no place in the life of a recovering addict. Failure to do so is one of the most common relapse factors in all stages of recovery.
Second, a healthy lifestyle is crucial during recovery, especially with depression. Incorporating proper diet and exercise routines is one of the best ways to fight off mental health and addiction.
There is even a saying in the medical community that if there were ever a pill that offered all of the same benefits as exercise, it would be the greatest advancement in medical history. Don’t underestimate the value of exercise on mental health.
Exercise and a healthy diet promote the regulation of hormones, endorphins, and neurotransmitters that are hindered by conditions like depression. When paired with a proper diet, depression has a difficult time developing.
Next, forming positive relationships is critical. If a person only sees their sponsors and therapists once a week, they need to fill in the rest of the gaps by spending quality time with loved ones who care about their sobriety.
Finally, doing things that encourage positive feelings is important to improve a person’s current mental health status, adapt to a sober lifestyle, and promote a healthy outlook on life. Picking up a hobby, learning a new skill, or simply getting outside has positive effects on mental health as well as addiction recovery.
One of the biggest hurdles during early recovery, especially shortly after rehab, is developing a positive outlook on life and learning to enjoy life while sober. That’s why positive interactions and activities are so important.
Find Help Today
It’s no surprise that the combination of depression and addiction is a serious danger to a person’s well-being and needs to be treated right away. If a loved one is suffering from a similar combination, then hopefully you now know what to do. The sooner you find help for them, the better.
Stay up to date with our latest addiction news and feel free to contact us with any questions about our programs.
References & Resources
13 remarkable health benefits of getting outdoors. TripOutside. (2021, December 3). Retrieved from https://www.tripoutside.com/health-benefits-of-getting-outdoors/
MediLexicon International. (n.d.). Hidden signs of depression: How to spot them and what to do. Medical News Today. Retrieved from https://www.medicalnewstoday.com/articles/325513
National Institute on Drug Abuse. (2020, July 10). Treatment and recovery. National Institute on Drug Abuse. Retrieved from https://www.drugabuse.gov/publications/drugs-brains-behavior-science-addiction/treatment-recovery
Toxic friendships & relationships. Jean Hailes. (n.d.). Retrieved from https://www.jeanhailes.org.au/news/toxic-friendships-relationships
U.S. Department of Health and Human Services. (2015, November 18). 10 percent of US adults have drug use disorder at some point in their lives. National Institutes of Health. Retrieved from https://www.nih.gov/news-events/news-releases/10-percent-us-adults-have-drug-use-disorder-some-point-their-lives